In this article:
- Healthcare at a distance
- Spike in usage of telemedicine
- Of those who have used telemedicine, nearly 3 in 4 did so for the first time during the pandemic
- For consumers not using telemedicine, would they find it useful?
- Pent up demand for telemedicine is high across the world, but particularly in these five countries
- Leveraging artificial intelligence in patient-provider interactions
- Opportunity gap
- People are enthusiastic about mobile messaging options, but adoption remains stubbornly low
Research from Sinch shows a dramatic shift in consumer behavior — away from public spaces and physical meetings to favor digital interactions. And in the healthcare sector, the transition is even more pronounced. Usage of telemedicine has surged 245% since the COVID-19 crisis began, and many expect these changes will outlast the pandemic, marking a permanent shift in health-seeking behavior.
Surveying 2,890 consumers across 14 countries, Sinch documents dramatic changes in behavior and pinpoints the features and solutions patients want most from their healthcare relationships. People now want virtual and mobile health experiences - if only the sector can sprint to deliver it.
Healthcare at a distance
People worldwide are avoiding physical spaces and gathering places, in favor of digital or virtual interactions. According to Sinch’s research, there is a strong indication that this trend will continue even after the pandemic is over. Fifty-eight percent say they will avoid crowds after COVID-19 has passed and 43% will stay closer to home. These figures signal profound changes in everyday life.
Not surprisingly, health-seeking behaviors have also been influenced by the pandemic. 39% say they currently use telemedicine, and of that share, the majority (71%) say they began using telemedicine during the COVID-19 crisis — marking a 245% increase.
Spike in usage of telemedicine
Of those who have used telemedicine, nearly 3 in 4 did so for the first time during the pandemic
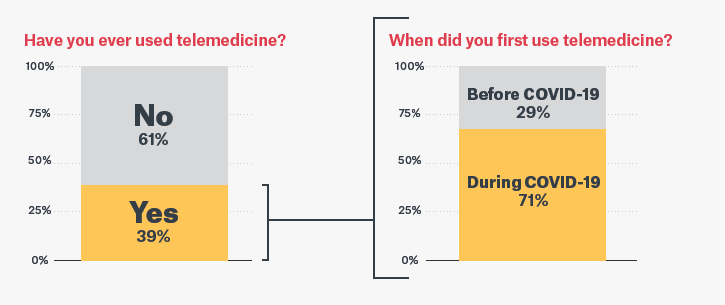
Even among those who do not use telemedicine, there is pent-up demand. Forty-two percent say they would like to use it but haven’t gotten around to it, and 17% say they would like to use it but their medical providers don’t offer it.
For consumers not using telemedicine, would they find it useful?
Pent up demand for telemedicine is high across the world, but particularly in these five countries
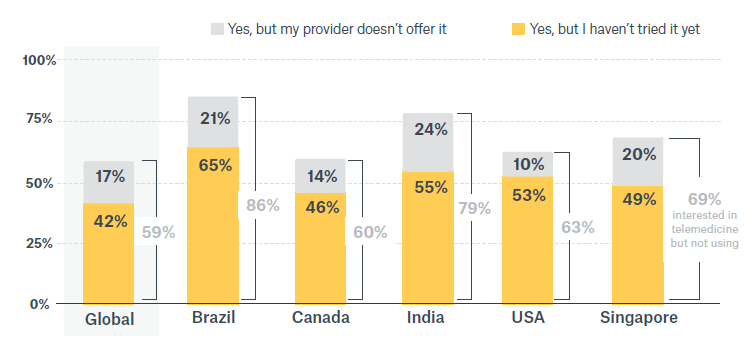
McKinsey’s recent study points out that even with this upsurge in usage, there is a massive amount of additional healthcare activity that can be delivered remotely. It estimates that in the U.S. alone, an additional $250 billion of the healthcare sector can be virtualized.
Leveraging artificial intelligence in patient-provider interactions
Medical visits aren’t the only area poised for disruption. For an individual patient, hundreds of interactions occur around the doctor-patient visit, from making and confirming appointments to filling out pre-visit assessments and monitoring physical symptoms. These can be done more efficiently — and even enjoyably — using mobile conversations powered by artificial intelligence.
In some cases, AI offers medical support to healthcare specialists; it does this by delivering patient surveys specific to a particular illness or disease and then giving healthcare providers a quantitative assessment of recommendations.
Mobile assessments are easy for patients to use, and help make medical appointments more efficient and effective.
And the research shows that consumers are ready to embrace these new formats, including using mobile messaging for many more healthcare interactions. For example, just 14% say they have assessed their health via mobile messaging, but 78% would find this useful. Thirty-six percent have used messaging to make an appointment, but 88% would like to do this.
The gap between current usage versus what patients find useful is what Sinch calls the opportunity gap. These are areas where healthcare companies and providers should focus their efforts to meet patients’ needs.
Opportunity gap
People are enthusiastic about mobile messaging options, but adoption remains stubbornly low
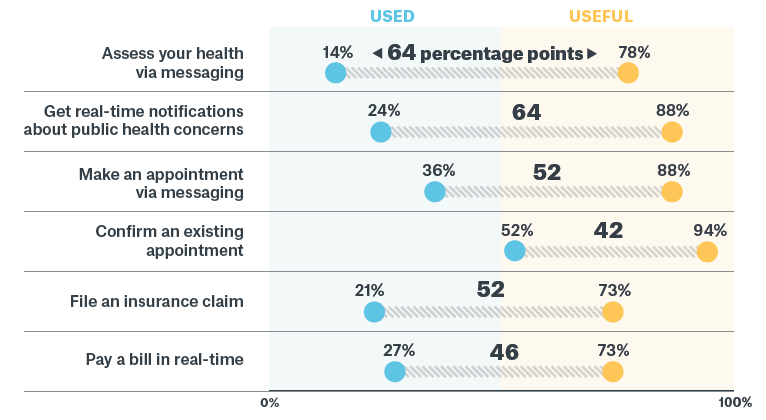
One of the biggest opportunity gaps is in public health messaging. Since the pandemic began, Sinch has provided digital communications infrastructure to governments and health authorities worldwide. The Sinch messaging ecosystem empowers health agencies to send out real-time public health notifications, and enables citizens to use mobile channels to make appointments for COVID-19 tests, schedule medical visits, and ask questions about symptoms without leaving the house. In Uruguay, for example, a government-sponsored app connects at-risk citizens with the tools they need to learn about COVID-19 and seek testing and treatment. Not only does it deliver health resources and send out test results, but the app also supports in-app video calling with clinicians to assess whether a sick individual should go to the hospital or quarantine at home. In Uruguay this app was downloaded 200,000 times in the first two weeks after release, pointing to the demand for mobile public health tools.
"Mobile healthcare tools like TelASK have also been a powerful solution during the pandemic because they provide a type of 'digital triage'", explains Anders Lenman, RTC Product Manager at Sinch. "TelASK, and solutions such as those used by the Uruguay government, identify citizens who are at highest risk, and connect them with the services they need, all while shielding other citizens from unnecessary exposure. Plus they can offer in-app video calls with providers, which can be very reassuring when an individual is fearful of visiting hospitals or other clinical settings."

The next generation of mobile healthcare
Even beyond routine, task-oriented interactions such as making appointments or filling out forms, healthcare companies and providers have an opportunity to use AI to support conversational healthcare.
While chatbots have been around for a few years, advances in natural language processing make them excellent channels to share health information and support patients. For example, CancerChat, a chatbot that operates through Facebook Messenger, is a resource for cancer patients and their families. It answers questions about treatment regimens, nutrition, and medication side effects — and in doing so, it allays fears when a patient feels most vulnerable. The chatbot also routes patients with more challenging questions and concerns to their providers.
Automated conversations can also help support employee safety — an application that’s been highly valuable for healthcare institutions during the pandemic. The University of Ottawa Heart Institute, for example, uses a daily screening questionnaire, completed via SMS, to assess symptoms and issue a “wellness pass” to enter the building. And government agencies are using solutions like TelASK to assess COVID-19 hotspots as well as point citizens to community testing and resources.
Chatbots can play an important role because they are always available and “on” for patients. The Sinch research shows people who use chatbots rate them as most effective concerning availability, privacy/anonymity, and speed.
As we shift to a post-COVID world, the healthcare sector faces an important reckoning. Alex Jadad, founder of the Centre for Global eHealth Innovation, University of Toronto, puts it this way: “The regulatory barriers that have held virtual health care back for all these decades were never justifiable. [COVID-19] is an opportunity to blow all these barriers away.”
The question now is “how far are we willing to go?” Given patients’ appetite for more virtual and mobile solutions, we believe the post-COVID era will be one of tremendous innovation.
Want to find out even more about how patients are using telehealth and mobile health applications?
Download Sinch’s latest industry report: Healthcare reborn.
Plus, find the entire series, Customer experience in a transformed world, here.



